- 800.809.7000
-
Carenet Health HQ
11845 Interstate 10 W
San Antonio, TX 78230












Americans have access to Carenet solutions
top Health Systems use our platforms
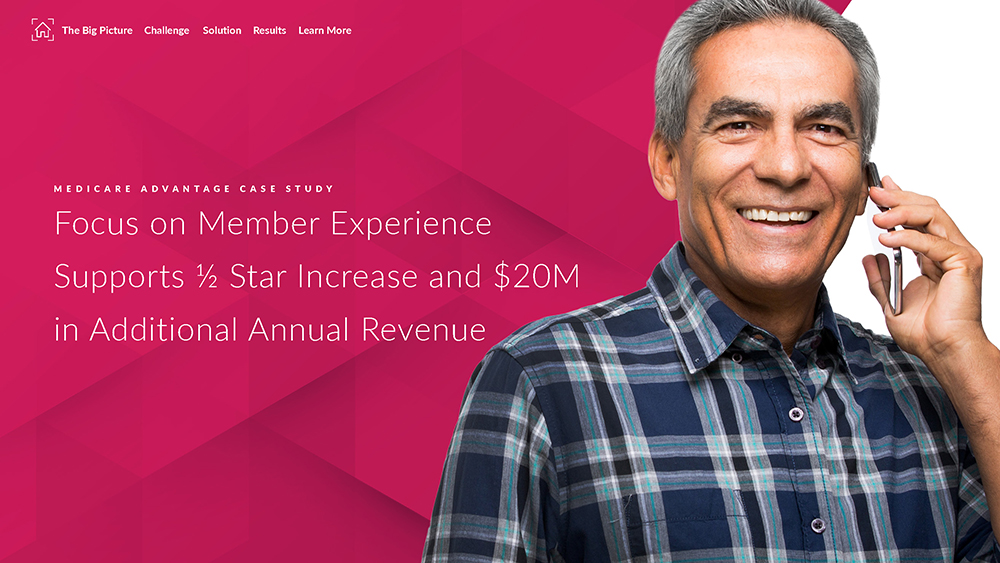
Our collaborative process begins with design thinking to help you define your priorities and ends with solutions that transform your business for the better.
Pinpoint key issues or opportunities that need to be addressed.

Analyze information to understand the context and implications of the identified issues.

Brainstorm potential solutions or ideas that address the interpreted needs creatively.

Develop and refine the imaginative ideas into actionable and novel solutions.

Critically evaluate the innovative solutions to ensure they meet the defined objectives and are feasible.

Execute the final solution, putting it into practice and monitoring its impact.